Last Updated on January 14, 2021. with family & friends to help keep them safe.
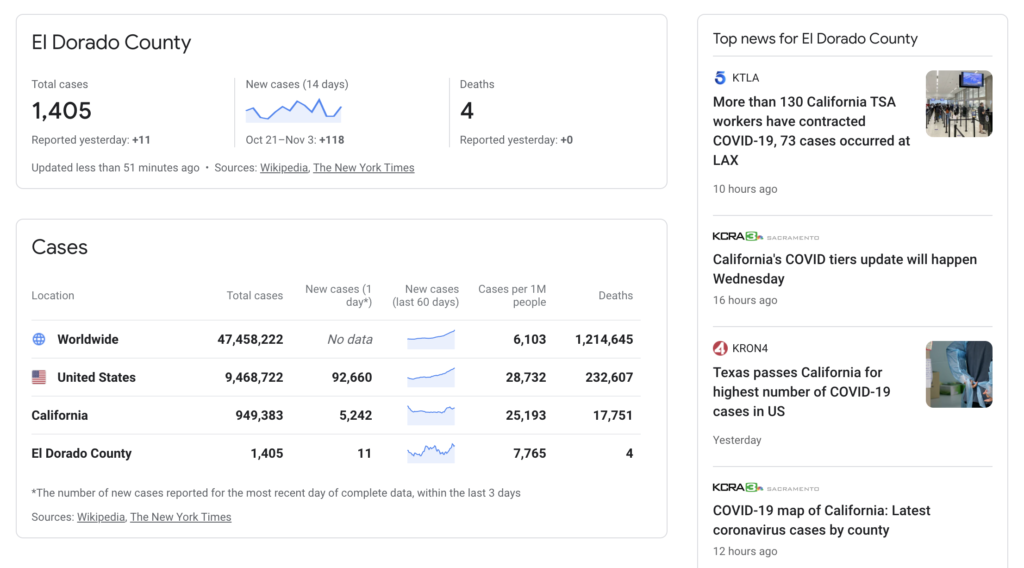
Source: Heavenly and Sierra at Tahoe are resorts located in El Dorado County – https://news.google.com/covid19/map
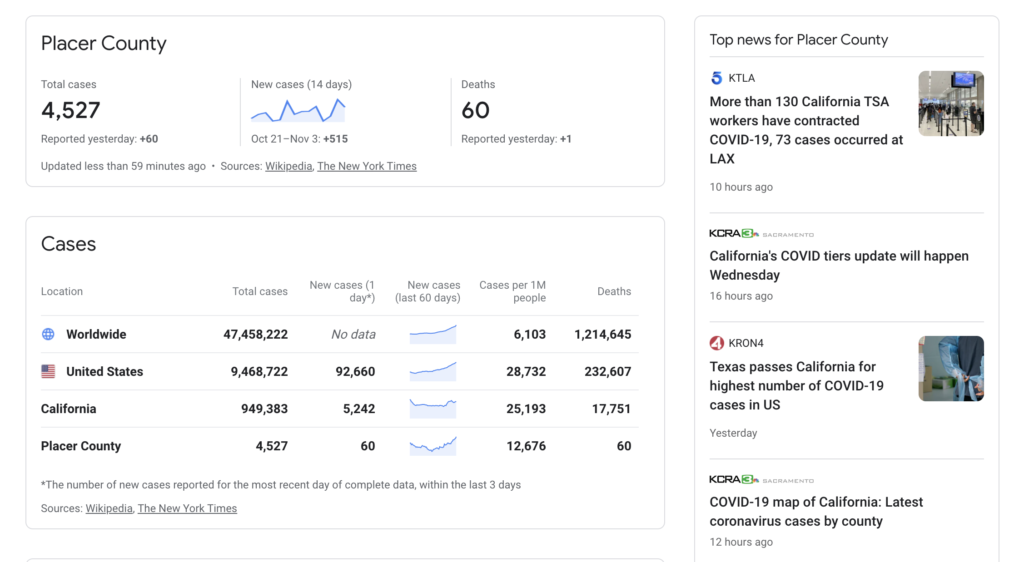
Source: Northstar, Squaw Alpine, Sugar Bowl are resorts located in Placer County – https://news.google.com/covid19/map
Check the current COVID case count for your county and CA’s Covid Tier assignments at
✔ https://news.google.com/covid19/map.
✔ Check El Dorado (South Tahoe).
✔ Placer County (North Tahoe).
*Remember to check your county’s COVID Tier and travel restrictions before you plan your trip. To ski, snowboard at Lake Tahoe resorts, advance reservations are required (no day of lift ticket sales available) because ski resorts have to limit resort’s visitors’ capacity as a Covid mitigation measure.
?Town of #Truckee has clear guidance on what is allowed during the 3 weeks of Stay at Home order; #Tahoe resorts R opened since #CA designated resorts as #outdoorrecreation. No overnight hotel stays or short term rentals less than 15 days allowed https://t.co/Js82eXbh50… #SF ⛷
— SnowPals.org SF, CA (@SnowPalsDotOrg) December 16, 2020
View a U.S. Map of COVID-19 cases
https://coronavirus.jhu.edu/us-map
Lodging Share During the Pandemic FREQUENTLY ASKED QUESTION (FAQ)A frequently asked question SnowPals.org get asked is..
Our group will be sharing a Lake Tahoe rental/ski lease lodge for the winter season and I’d like to ask you what safety measures should I implement during COVID-19 to prevent my friends and family from getting infected with the coronavirus (which will ruin everyone’s enjoyment of snow sports this winter)?
Great question and an important one because although deaths related to Covid19/coronavirus have decreased significantly, however, the rate of infection is still rising quickly as the winter months flu season starts and there is no united or coherent federal leadership and guidance on Covid prevention as states issue various guidance from no masks required to masks mandated.
Before we delve into safety measure tips, let’s first examine the impacts of coronavirus..
Long-term effects of COVID-19
According to the Mayo Clinic, long-term effects of COVID-19 (coronavirus) includes problems with mood swings and fatigue..
Many people who have recovered from SARS have gone on to develop chronic fatigue syndrome, a complex disorder characterized by extreme fatigue that worsens with physical or mental activity, but doesn’t improve with rest. The same may be true for people who have had COVID-19. – Mayo Clinic
Costs for a Hospital Stay for COVID-19
“FAIR Health estimated the costs based on ICD-10 procedure codes and revenue codes associated with flu and pneumonia (lung inflammation caused by infection). We analyzed data from our database of over 30 billion private healthcare claim records, the largest such repository in the country. We found the average charge per COVID-19 patient requiring a hospital stay to be $73,300. That charge is the estimated cost for a patient with no health insurance. It’s also the cost for a patient seeing an out-of-network provider and whose health plan has no out-of-network benefit.
The average estimated in-network amount per privately insured patient is lower: $38,221. The in-network amount is the amount that the providers in the plan’s network have agreed to accept as full payment. It includes both the amount the plan pays and the amount the patient pays. The amount the patient pays is based on the cost-sharing provisions of the plan.
These numbers are useful to know to help you understand how much the COVID-19 pandemic is costing our country. But it’s also important to know that they’re not the actual amount you’re likely to have to pay if you or someone in your family gets COVID-19. If you have insurance, your costs will be determined by the cost-sharing terms of your health plan. If you don’t have insurance, your costs will vary based on your specific case. And you may be able to negotiate a lower amount with your providers.” – https://www.fairhealth.org/article/costs-for-a-hospital-stay-for-covid-19
Updated #COVID19 #SARSCoV2 case timeline, with references cited and other improvements. PDF with embedded links to each reference can be downloaded here: https://t.co/CMaCJNi5bu https://t.co/kOZ6BsEZj1 pic.twitter.com/AZm3EacgNf — David R. Liu (@davidrliu) June 11, 2020
Symptoms of coronavirus/COVID
COVID-19 affects different people in different ways. Infected people have had a wide range of symptoms reported – from mild symptoms to severe illness.
Symptoms may appear 2-14 days after exposure to the virus. People with these symptoms may have COVID-19:
“COVID-19 is a respiratory condition caused by a coronavirus. Some people are infected but don’t notice any symptoms. Most people will have mild symptoms and get better on their own. But about 1 in 6 will have severe problems, such as trouble breathing. The odds of more serious symptoms are higher if you’re older or have another health condition like diabetes or heart disease.
Here’s what to look for if you think you might have COVID-19.
Common Symptoms
Researchers in China found that the most common symptoms among people who were hospitalized with COVID-19 include:
Fever: 99%
Fatigue:70%
A dry cough: 59%
Loss of appetite: 40%
Body aches: 35%
Shortness of breath: 31%
Mucus or phlegm: 27%
Other symptoms may include:
Sore throat
Headache
Chills, sometimes with shaking
Loss of smell or taste
Congestion or runny nose
Nausea or vomiting
Diarrhea
Look for emergency warning signs for COVID-19. If someone is showing any of these signs, seek emergency medical care immediately:
Trouble breathing
Constant pain or pressure in your chest
Bluish lips or face
Sudden confusion
Inability to wake or stay awake
Bluish lips or face
You need medical care as soon as possible. Call your doctor’s office or hospital before you go in. This will help them prepare to treat you and protect medical staff and other patients.
Strokes have also been reported in some people who have COVID-19. Remember FAST:
Face. Is one side of the person’s face numb or drooping? Is their smile lopsided?
Arms. Is one arm weak or numb? If they try to raise both arms, does one arm sag?
Speech. Can they speak clearly? Ask them to repeat a sentence.
Time. Every minute counts when someone shows signs of a stroke. Call 911 right away.
Lab tests can tell if COVID-19 is what’s causing your symptoms. But the tests can be hard to find, and there’s no treatment if you do have the disease. So you don’t need to get tested if you have no symptoms or only mild ones. Call your doctor or your local health department if you have questions.
Call your medical provider for any other symptoms that are severe or concerning to you.” – WebMD
Is COVID-19 similar to the common cold?
“Coronaviruses usually cause mild to moderate upper-respiratory tract illnesses, like the common cold. However, SARS-CoV-2 can cause serious illness and even death. Why people’s COVID-19 symptoms vary so greatly isn’t fully understood.
What is the difference between the flu and COVID-19 regarding how long it takes to develop symptoms?
Flu
Typically, a person develops symptoms anywhere from 1 to 4 days after infection.
COVID-19
Typically, a person develops symptoms 5 days after being infected, but symptoms can appear as early as 2 days after infection or as late as 14 days after infection, and the time range can vary.
If you suspect you have the above symptoms, take a self-assessment.
The New York Times reported:
The U.S. recorded more than 90,000 new coronavirus cases yesterday, a new daily high. That’s more than one new case every second, The Times’s Mike Baker notes.
Stephanie Ruhle On COVID-19 Diagnosis: I Did All The Right Things, But I Still Got The Virus | MSNBC YouTube Video:
Some good news: Survival rates among severe virus patients are improving. At N.Y.U.’s hospital system, the death rate dropped to 8 percent in August, from 26 percent in March.
COVID-19 VACCINE PROGRESS UPDATE
READ the latest news on the progress of an effective COVID-19 vaccine (link opens in new window to show vaccine news update)
Coronavirus vaccines 101: What you need to know
What is a vaccine?
How will vaccines for the new coronavirus work?
Are these vaccines safe?
If a vaccine is working, how soon will a person who gets it be protected?
Why bother with a vaccine if we can just slow-burn until herd immunity?
Why do I keep hearing people talk about vaccines that are “safe and effective?”
How soon will coronavirus vaccines be ready?
How soon could I get a vaccine?
What’s a clinical trial? And what are these trial “phases” anyway?
Who will get vaccines first?
Will coronavirus vaccines have side effects?
UC HEALTH answers the above questions in a clear and easy to understand explanation 😉 – https://www.uchealth.org
Preventative Safety Measures
To prevent Covid infection/transmission, aside from keeping social distancing, our recommendations are sourced from leading career doctors and scientists:
(1) Agree on a set of safety protocols but most importantly, all members of the ski lease must stick to following them without fail. As a group collectively agree to and implement ‘preventive health measures like frequent hand washing, physical distancing, and wearing a mask when going out in public, to help protect themselves and to reduce the chances of spreading the infection to others.’ – Read Harvard Health’s Recommendations
Have available at all corners of the ski cabin/ski lease from ski lodge entrances to bedrooms, hand sanitizer bottles readily available to use in all community areas/located by high touch shared items, microwave, door knobs, etc.
Work collectively means it’s critical to keep everyone in the loop and to communicate clearly with daily updates especially if a member have recently been in high risk situations/exposed to Covid. Make use of Group Coordination and Collaboration Calendars and Tools to keep everyone in the loop.
? #SF #CA: #60Minutes on YOUTUBE ? — SnowPals.org SF, CA (@SnowPalsDotOrg) December 23, 2020
How the Pfizer-BioNTech COVID-19 was made.. in the middle of the video, observe how doctors wear not only face masks ? but also face shields to protect their eyes: Virus ? infection routes via nose, mouth & eyes ➡️ https://t.co/B7sQs8gDL8 https://t.co/vphAeD7NgQ pic.twitter.com/ihAWqt3dBM
(2) Use HEPA air purifiers – one for each bedroom, one for the living, dining room area which can remove up to 99.97% of bacteria, molds, and viruses. ‘And long enough exposure to the UV light in an air purifying device can disable some viruses, including COVID-19.’ – https://www.mdanderson.org.
Find an AHAM (Association of Home Appliance Manufacturers) Certified Room Air Cleaner. Performance is key when choosing the right air filter for your home. – https://ahamverifide.org/directory-of-air-cleaners/
(3) Buy and use the best available N95 masks, CDC approved, NIOSH certified N95 masks
(4) Check your central air/heating system to see how air is directed/identify air flow vents and see how air is directed into each room of your home. If your air vent is blowing air from mid-torso to head level, consider having a qualified handyman or AC/Heating specialists install air flow duct accessories that will direct the outbound air directly to the ground. Why? It has been shown that air flow directly to the ground is key in preventing virus transmission by directing the air to the ground instead of to the torso and head level where infected asymptomatic person(s) virus exhalation can be captured and spread by the air flow of the AC/Heating unit.
See screen-capture photo of how airflow on an airplane effectively does this:
Effective use of HEPA certified air purifiers to eliminate coronavirus:
Safe travels start with science
“Studies show COVID-19 exposure risk is minimal when air filtration systems and masks are in use
The latest research is showing that aircraft cabins are among the safest of public indoor environments. According to a recent study conducted by the U.S. Department of Defense (DOD), the risk of COVID-19 exposure on board our planes is almost zero thanks to advanced air filtration systems, required mask-wearing and diligent cleaning protocols.
Since airlines began putting these measures in place in spring 2020, “there has been little evidence to date of onboard disease transmission,” according to researchers at Harvard T.H. Chan School of Public Health. Their report notes that when the “highly effective” ventilation systems are running from boarding until deplaning, which is our practice at United, the risk of exposure falls below that of activities like grocery shopping and dining out.
And even when the plane is full, on average only 0.003% of infected air particles could enter the breathing zone of seated, masked passengers, according to the DOD study.”
Reference:
Read Harvard’s study
Read U.S. Department of Defense’s study
How using a humidifier to maintain your house’s humidity at 40-60% is optimal in reducing the risk of viral infections in the common flu and Coronavirus infections:
? “Maintaining proper #humidity reduces coronavirus infection risks. This is part of a project involving top researchers from around the world & #AI analyzing 200,000 COVID-19 papers” - Read more at #HarvardUniversity’s @SITNBoston | ⛷? =@SnowPalsDotOrg pic.twitter.com/HZJ5N4hJQC — SnowPals.org SF, CA (@SnowPalsDotOrg) December 24, 2020
How taking Vitamin D supplements during the winter months help to boost your immune response to viral infections including Covid-19?
YouTube Interview with Professor Roger Seheult, MD; Dr. Seheilt explains the important role Vitamin D may have in the prevention and treatment of COVID-19. Dr. Seheult illustrates how Vitamin D works, summarizes the best available data and clinical trials on vitamin D, and discusses vitamin D dosage recommendations.
Roger Seheult, MD is the co-founder and lead professor at https://www.medcram.com
He is an Associate Professor at the University of California, Riverside School of Medicine and Assistant Prof. at Loma Linda University School of Medicine
Dr. Seheult is Quadruple Board Certified: Internal Medicine, Pulmonary Disease, Critical Care, and Sleep Medicine
#CA During #winter months when most spend a bulk of their time indoors, critical to TAKE #VITAMIND supplements to boost your immune system to fight off viral infections: flu & coronavirus? — SnowPals.org SF, CA (@SnowPalsDotOrg) December 24, 2020
“Vitamin D deficiency found in over 80% of COVID-19 patients” - https://t.co/kWs7Mbh44E https://t.co/gEv7k9LR2L pic.twitter.com/rD9GKOZrP9
How maintaining regular exercise helps to boost your body’s immune system?
?❄️⛷? #SanFrancisco Bay Area #SiliconValley CA: got your daily #Vitamin E? E as in EXERCISE #optoutside OUTDOOR RECREATION @SnowPalsDotOrg ?➡️ “Immunometabolism and Covid-19: Could Lifelong Exercise Training Have a Protective Effect?” - @HapresL https://t.co/EktMVzhc9o… “ https://t.co/hVKkzKqdD4 pic.twitter.com/PREAwBvB7L — SnowPals.org SF, CA (@SnowPalsDotOrg) December 24, 2020
How effective are masks in terms of preventing Covid infection/transmission?
Mask Standards and Effectiveness Bottom Line
New study from Ueki et al. with live airborne #SARSCoV2 virus confirms
1) Masks worn by infected ppl reduce #coronavirus transmission.
2) Masks worn by healthy ppl protect themselves from infection.
3) N95 mask>surgical>cloth>no mask
(1/2)https://t.co/9V0R5YoiYX
Note log scales. pic.twitter.com/4XoD4K6etF— David R. Liu (@davidrliu) October 24, 2020
– Single use masks (normally one layer, very thin) are typically only effective at capturing larger dust particles, but can do so fairly well.
– Surgical mask standards have higher requirements for capturing virus-sized (0.1 micron) particles, however they vary by region.
– Pollution masks (respirators) typically capture >90% of virus-sized particles. You can use the rating system in the table above to see the exact proportion each certification requires. This includes ratings such as N95, KN95, FFP1, FFP2 and FFP3. – https://smartairfilters.com/en/blog/comparison-mask-standards-rating-effectiveness/
COVID-19: Droplet or Airborne Transmission? Penn Medicine Epidemiologists Issue Guidance
CDC updates guidance on aerosolized COVID-19 spread
According to #Taiwan virology expert opinion, he did not understand why the West puts so much emphasis on #SocialDistancing but not #N95 #Masks , regular masks don’t protect the wearer. — Winston T (@WinstonTsao) October 30, 2020
Where do you buy your N95 NIOSH certified masks?
https://www.idcband.com/en-us/respirator-face-masks/
* Disclosure: SnowPals.org does not get any kick-backs/commission for any of the links in this featured article btw.
Comparison of Mask Standards, Ratings, and Filtration Effectiveness – https://smartairfilters.com
(5) Collectively agree to get Covid tested 24-48 hours of first meetup at the ski lease cabin(in the meantime, shelter in place until you get your test result); share test results prior to first meetup, after which all ski lease members keep a contact journal of daily activities and share any incidents of concern. Keeping a social contact and activities journal can be time consuming but if it means everyone in the ski lease is more mindful of his/her contacts and activities they engage in that can be cause for concern/considered high risk, can then be shared among all members. Communication is key. Find free Covid testing near you (opens in a new window using Google search).
Which ski lease group did the most research and analysis on best practices for Covid safety protocols?
http://www.snowpals.org/leases/covid-adjusted-south-lake-tahoe-ski-lease-share/
Feel free to contact Mike (the ski lease organizer – see contact link in above URL) to share tips.
Additional Reading
✔ Tahoe Ski Season Survey & Insights
✔ Read about specific coronavirus safety measures Tahoe resorts are implementing to keep staff and visitors safe
✔
CNN TRAVEL COVERS skiing in times of COVID..the ‘lodge’
Flexibility is key
Ticket to ride
Planning for the worsthttps://www.cnn.com/travel/article/skiing-seasons-changes-coronavirus
?
✔ Keep track of United States vs California’s COVID19 cases as winter flu season starts.
Johns Hopkins Coronavirus Resource Center: Homecoronavirus.jhu.edu
Johns Hopkins experts in global public health, infectious disease, and emergency preparedness have been at the forefront of the international response to COVID-19 pandemic.
✔ Who’s going to pay for Covid-19 treatment?
✔ Estimating potential spending on COVID-19 care, a report by Brookings Institute www.brookings.edu
✔ What is the trend for snow sports during these times?
✔ What did New Zealand do to control COVID-19 to successfully get to zero new infection; how did they managed to keep it that way, and what we can learn from them?
Please feel free to with friends and family ♥ to keep them safe 😉
?❄️☃️⛷?⛸
Engage in Critical Thinking
– Critical to democracy & survival of citizens of these United States of America
TOTALLY UNDER CONTROL – Official Documentary Trailer On-demand on Hulu
On Demand October 13
On Hulu October 20On January 20th, 2020 the US and South Korea both discovered their first cases of COVID-19. However, 9 months later, the novel Coronavirus has claimed the lives of over 200,000 Americans and caused staggering economic damage, while in South Korea, there were no significant lockdowns and, in an urbanized population of 51 million, only 344 lives have been lost. Where did we go wrong? As the presidential election nears, Americans are increasingly enraged by a lack of clear leadership, endemic political corruption and left to wonder how did the wealthiest and most powerful country in the world manage to fail so thoroughly in its response to a global pandemic?
Academy Award-winning filmmaker Alex Gibney, directing with Ophelia Harutyunyan and Suzanne Hillinger, interrogates this question and its devastating implications in Totally Under Control. With damning testimony from public health officials and hard investigative reporting, Gibney exposes a system-wide collapse caused by a profound dereliction of Presidential leadership.
It will be a generation before we know the full extent of the damage wrought by this pandemic, but Totally Under Control will stand as the definitive account of the Trump administration’s incompetence, corruption and denial in the face of this global pandemic.
Senate GOP disavowed their oaths to let Trump off the hook during the Impeachment Trial, Trump takes no responsibility for the Covid response & Grassley is doing nothing about an unreasonable dismissal of an IG>Trump is a dictator with GOP supporthttps://t.co/Yvu5XShVZY — Mel Lin (@M3ll1n) May 18, 2020